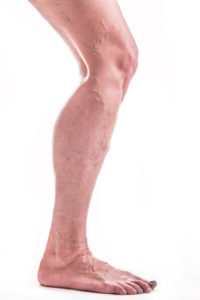
 Sclerotherapy is a medical procedure that’s beneficial in treating many types of blood vessel problems, vascular malformations and some lymphatic system issues. A medication or solution is injected into a vessel or other area to cause it to shrink or close. It can used for vascular and lymphatic malformations in children and young adults. In adults, it is most often used as a treatment for varicose veins, spider veins and even painful hemorrhoids.
Sclerotherapy is a medical procedure that’s beneficial in treating many types of blood vessel problems, vascular malformations and some lymphatic system issues. A medication or solution is injected into a vessel or other area to cause it to shrink or close. It can used for vascular and lymphatic malformations in children and young adults. In adults, it is most often used as a treatment for varicose veins, spider veins and even painful hemorrhoids.
Along with surgery, laser ablation, radiofrequency treatment and other methods, sclerotherapy is one recommended method of treating spider veins and sometimes varicose veins and vein malformations (medial professionals see how to offer Sclerotherapy treatment).
In the case of ultrasound-guided sclerotherapy, duplex ultrasound is used to see the vein so the physician can monitor and deliver the medication injection with complete accuracy. This type of ultasound-guided procedure when used along with microfoam sclerosants has proven more effective in reflux control than other methods. Some researchers have, however, indicated that sclerotherapy is not the right choice for veins with reflux at the saphenous junction or with axial reflux.
History
For more than 150 years, sclerotherapy has been used for treating spider and varicose veins. As you might expect, techniques have changed and evolved greatly with time and technological advancements. Today’s techniques involve ultrasound guidance and foam solutions that provide better and more accurate results than ever before.
The first recorded sclerotherapy effort was performed by Zollikofer in 1682 in Switzerland. This practitioner injected a sort of acid into a vein to cause a thrombus formation. Both Cassaignaic and Debout reported having success with treating varicose veins with a perchlorate or iron in 1853. In 1854, Desgranges cured 16 varicose vein cases with injections of iodine and tannin.
Twelve years before that, in 1844, Madelung invented the saphenous vein stripping procedure, temporarily causing a loss of interest in this procedure. Early sclerotherapy procedures had high rates of side effects, and sclerotherapy was all but abandoned by 1894. As surgical techniques improved and anesthetics got better too, stripping became preferred over sclerotherapy.
Work to develop alternative sclerosants continued in the early 20th century. Perchlorate of mercury and carbolic acid were tried and worked well, but unexpected and unacceptable side effects caused these solutions to be abandoned. Sicard and some other French doctors developed the idea of using sodium carbonate and later sodium salicylate as sclerosants after World War I. Quinine was also effective in the early twentieth century. In 1929, Coppleson advocated the use of sodium salicylate and quinine.
Work to improve the technique and develop better sclerosants continued during and after the Second World War. Particularly important was the development of STS in 1946, the product still widely used for sclerotherapy. In the 1960s, George Fegan reported that he treated more than 13,000 people with sclerotherapy, advancing the technique significantly and focusing on vein fibrosis rather than thrombosis, controlling significant reflux points and emphasizing how important adequate compression is to the treated leg in the days after treatment. In mainland Europe, the procedure gained acceptance during that time. It was not well understood or accepted in the United States or England at that time, however, something that is still the case in some under-educated subsections of the medical community.
The invention of duplex ultrasound in the 1980s was the next development in the evolution of sclerotherapy. A decade later, the two practices were integrated. Knight was an early advocate for this new way of doing sclerotherapy and presented it at some conferences in the United States and Europe. Thibault wrote the first paper on the topic to be published in a peer-reviewed journal.
Cabrera and Monfreaux contributed to the use of foam sclerotherapy, and Tessari developed a three-way tap method for foam production that further impacted positively the treatment of large varicose veins with this procedure.
Methodology
Unwanted veins are injected with a special solution that causes them to quickly shrink, close off and eventually dissolve over the coming weeks or months as part of the body’s natural healing process. Sclerotherapy is considered non-invasive and can often be completed in 10 minutes or so. For the patient, downtime is minimal, if any, and therefore much shorter than with invasive vein surgery.
For getting rid of larger spider veins and small to moderate varicose veins, this procedure is the most commonly used and is preferred over laser treatment. Several injections of sclerosant are shot into abnormal veins of the leg. Once the leg is properly treated, the leg is compressed with a compression bandage or a compression stocking. Some kind of compression treatment is usually worn for one to two weeks following treatments. Patients are encouraged to walk to aid in healing but discouraged for strenuous and aerobic activities. In many cases, two or more treatments several weeks apart are necessary for complete results.
The procedure can also be done using foam sclerosants and the use of ultrasound guidance when larger varicose veins, including the small and great saphenous veins, are involved. First, a map of a patients varicose veins is made using the ultrasound technology, then the appropriate veins are injected while ultrasound is used to guide the procedure. Ultrasound allows the doctor to see the sclerosant going into the vein, and as many veins as necessary can be treated. Later, ultrasound scans are done during follow-up appointments to confirm that the veins are properly closed. Residual problem veins can be located and treated during this appointment.
Foam Sclerotherapy
Foam sclerotherapy involves injecting a foamy sclerosant into a blood vessel using a syringe. This drug is usually polidocanol or sodium tetradecyl sulfate and is mixed with air, carbon dioxide or another gas inside the syringe using a mechanical pump, effectively increasing the area of the drug coverage. Foam is more effective than liquid in causing the desired sclerosis — or thickening of the blood vessel and sealing of the blood flow. The foam does not mix with the blood within the vessel and actually does a good job of displacing it, reducing dilution that can cause the sclerosant not to work very well. This means the foam can be used in longer and larger diameter veins. There is a thick, toothpaste-like version of a foam sclerosant available that has revolutionized the treatment of varicose veins, vein malformations and Klippel Trenaunay syndrome.
Clinical Observations
In 1996, a study by Kanter and Thibault noted a three-quarters success rate after 24 months from sclerotherapy with a 3 percent solution used to treat saphenofemoral junction and great saphenous vein incompetence. Further, Padbury and Benveniste determined that sclerotherapy guided by ultrasound is effective for treating all sizes of varicose veins and leads to improved quality of life as well as high patient satisfaction.
A review of medical literature by the Cochrane Collaboration determined that there is evidence to support the current use of sclerotherapy in today’s clinical practices for recurrent varicose vein issues following surgery. A second review by the same organization concluded that this procedure has short-term benefits over surgery but that surgery works best in the long term, in many cases. Sclerotherapy was determined to be best in terms of success, complication rates and cost after a year, but surgery performed better over a five-year period. These reviews did not have entirely good data upon which to rely, however.
A Health Technology Assessment showed that this procedures offers fewer benefits than surgery but is to be expected to provide some benefit in varicose veins that do not have reflux from the sapheno-femoral or sapheno-popliteal junctions. It did not include a study of the benefits of surgery compared to sclerotherapy in varicose veins with this type of reflux.
In 2003, the European Consensus Meeting on Foam Sclerotherapy determined that foam sclerotherapy allows a practitioner with the right training and expertise to treat large veins effectively. A second meeting in 2006 has also been published.
Potential Complications
Complications are rare but can occur. These include vein thromboembolism, allergic reactions, skin necrosis, thrombophlebitis, redness and hyperpigmentation of the area around where treatment is performed.
When the sclerosant is properly injected into the vein, no damage should be expected to surrounding skin. When the solution is injected incorrectly and not within the vein, necrosis and scarring can happen. Necrosis is rare, but it can have devastating cosmetic impact and take months for complete healing. It is even more rare with dilute STS than with a 3 percent solution. Skin blanching is common with STS when used in small artery branches. Tiny red vessel development at the surface near injection can happen and may require treatment later with a laser or additional sclerotherapy.
The majority of complication happen because of an inflammatory reaction to the soluton in the area of the injection site. There can also be systemic complications that aren’t well understood. These happen when the drug in the solution moves through the veins and to the heart, brain or lungs. One report links strokes with foam sclerotherapy treatment. Additional reports have determined that bubbles from the solution rapidly travel to the lungs, brain and heart, but the significance of this fact is not yet known or understood.
Sclerotherapy is an approved treatment in the United States and is also approved in many other nations around the world. While this fact alone does not prove that it is safe, it has been widely used and widely studied for decades.

Why not revitalize your practice with Botox Training?








